The Desk Job Syndrome: How Sitting All Day Is Quietly Choking Your Pelvic Circulation

You probably don't think about your pelvis while you're grinding through back-to-back meetings, staring at spreadsheets, or commuting in rush-hour traffic. But your body is thinking about it — and not in a good way. Every hour you spend planted in a chair is an hour your circulatory system is fighting geometry.
The pipes that supply blood to your lower body get compressed, restricted, and ultimately underserved. Over time, that quiet daily insult adds up to something you'll notice in the gym, in the bedroom, and in the mirror.
This isn't a panic piece. It's a clear-eyed look at what chronic sitting does to pelvic blood flow, why it matters more than most men realize, and what you can do about it before the damage becomes a pattern.
"Every hour you spend planted in a chair is an hour your circulatory system is fighting geometry."
— Marcus AlcottThe Anatomy of the Problem
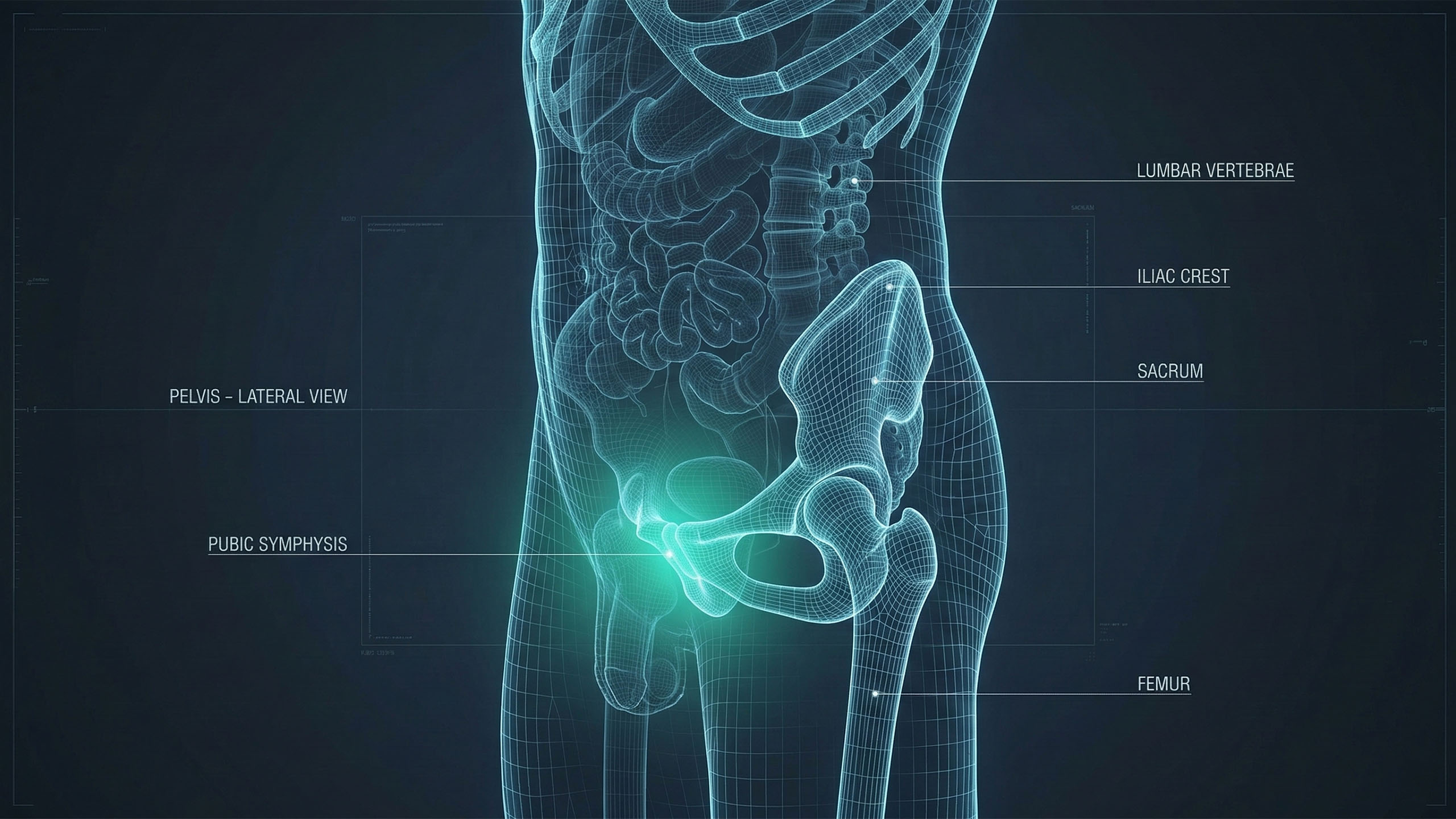
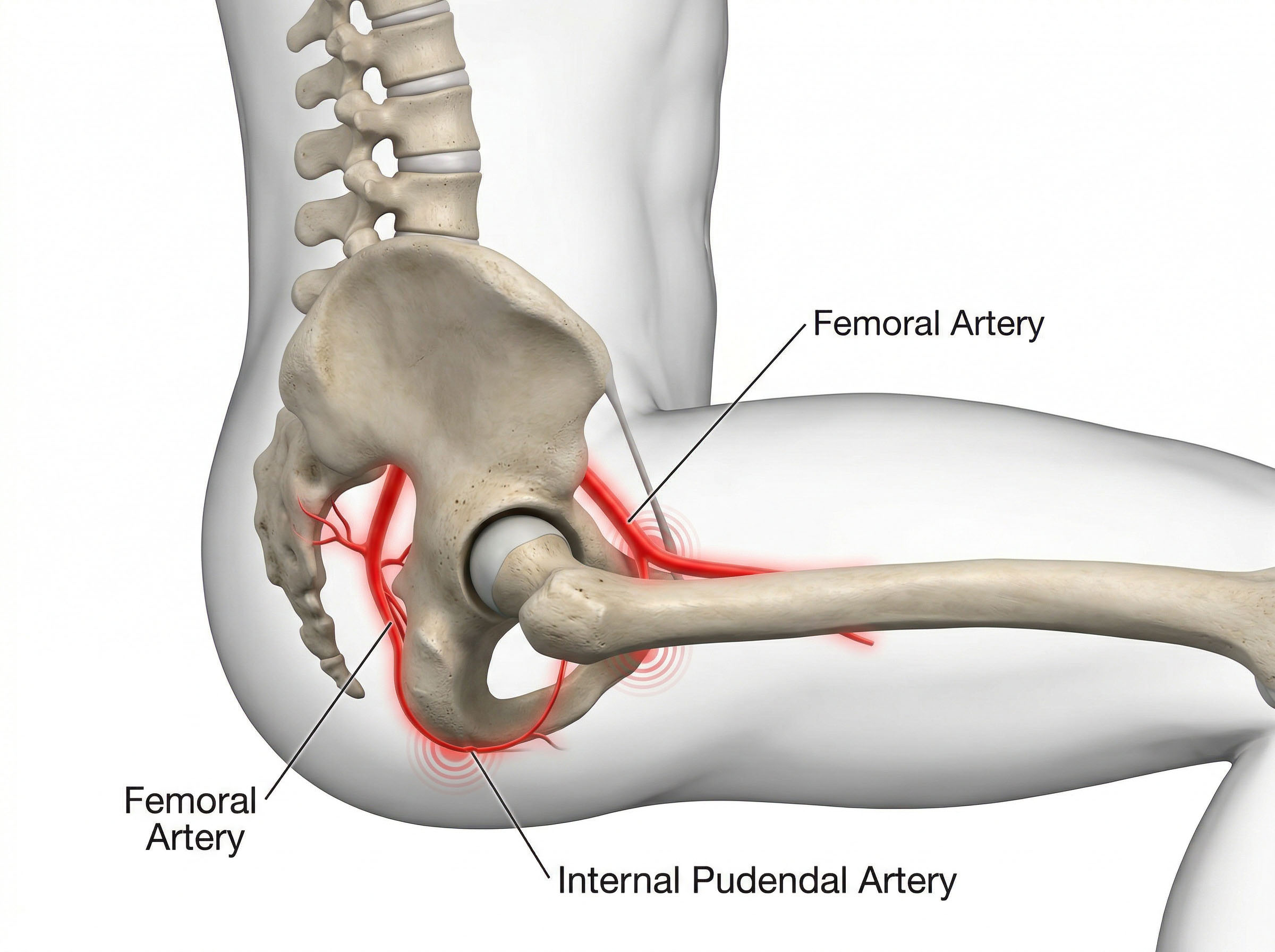
Your pelvis is one of the most vascular regions in the male body. The internal pudendal artery, the femoral artery, the iliac vessels — these are major highways, and they all run through or near the pelvic floor. When you sit, particularly in a slouched or forward-tilted posture with hips flexed past 90 degrees, several things happen mechanically that restrict flow along these routes.
First, the femoral vessels — the primary supply lines to your thighs and lower body — get pinched where they pass through the inguinal region. Think of kinking a garden hose. Flow doesn't stop entirely, but pressure drops and volume decreases. Second, the perineum (the floor of the pelvis, between your sits bones) absorbs direct compressive force from the chair seat. The pudendal nerve and artery run right through this tissue. Sustained compression here reduces both nerve signal quality and arterial blood supply to the genitals.
Research from the European Association of Urology has documented that prolonged perineal pressure — the kind generated by office chairs, especially poorly designed ones — correlates with reduced penile blood oxygenation. This isn't theoretical; it's measurable with Doppler ultrasound in clinical settings. The mechanism is straightforward: compress the supply line, reduce the delivery, observe the downstream effects.
ℹ︎ Did You Know?
The average office worker sits for 9 to 11 hours per day when you factor in commuting, desk work, and evening screen time. That's more time sedentary than the average person sleeps. Your circulatory system was not built for this load — anatomically, the human body was designed around roughly 4–5 hours of sitting per day in a hunter-gatherer context.
More Than Just Blood Flow
Blood flow is the starting point, but the downstream effects branch out further than most men expect. Healthy erectile function depends on the rapid, high-volume delivery of blood into the corpus cavernosum — the spongy erectile tissue inside the penis. That delivery requires healthy arterial walls, good endothelial function (the inner lining of your blood vessels), and a nervous system capable of triggering dilation on demand.
Chronic sitting undermines all three. Here's how:
| Mechanism | What Happens | Downstream Effect |
|---|---|---|
| Femoral compression | Vessels kinked at hip crease | Reduced blood volume to lower body |
| Perineal pressure | Pudendal artery & nerve compressed | Decreased penile oxygenation |
| Endothelial stress | Low shear stress + systemic inflammation | Reduced nitric oxide production |
| Pelvic floor inhibition | Muscles switch off, lose tone | Impaired venous pump, poor drainage |
| Posterior chain tightening | Hip flexors shorten, lumbar tilts | Altered pelvic posture, nerve impingement |
Endothelial function deserves special mention. The endothelium is the single-cell layer lining your blood vessels. It regulates vascular tone, clotting, and inflammatory response. Critically, it produces nitric oxide (NO) — the same molecule that triggers smooth muscle relaxation and blood vessel dilation during arousal. Sitting for long, unbroken stretches produces low shear stress on vessel walls, and shear stress is one of the primary signals that keeps endothelial cells healthy and NO production up. Remove the signal; production drops. This is one of the reasons sedentary men show measurable declines in vascular responsiveness even when other health markers look fine on paper.
The Testosterone Angle Nobody Talks About
There's another variable at play that gets less airtime: testicular temperature. The testes need to stay approximately 2–4°C cooler than core body temperature to produce testosterone and sperm efficiently. It's the reason they're housed outside the body in the first place. When you sit for hours, you trap heat in the scrotal region. The thighs press inward, clothing compresses, and the natural thermoregulatory mechanism — the cremaster muscle raising and lowering the testes to manage temperature — is overridden by sustained thermal load.
Elevated scrotal temperature has been associated in research with reduced sperm motility and morphology. For testosterone production, the data is more complex, but chronic heat stress on the testes is not something the male endocrine system handles with grace. It's one more way that sitting quietly erodes the conditions needed for peak male physiological function.
▶ Key Mechanism: The Nitric Oxide Connection
Nitric oxide (NO) is one of the most critical molecules in male vascular health. Produced by endothelial cells lining blood vessels, it triggers the relaxation of smooth muscle walls — allowing vessels to dilate and fill with blood. Exercise, dietary nitrates (from foods like beets, leafy greens, and pomegranate), and adequate shear stress on vessel walls all stimulate NO production. Prolonged sitting reduces shear stress, which directly suppresses this mechanism. Without adequate NO signaling, vascular response is slower, weaker, and less reliable — regardless of what's happening hormonally.
How Long Is Too Long?
There's no perfectly clean threshold, but the research consistently points to 30–60 minutes of continuous sitting as the point where measurable vascular changes begin. A study published in Medicine & Science in Sports & Exercise found that a single bout of 3 hours of sitting significantly reduced femoral artery flow-mediated dilation in young, healthy men — and that a single 10-minute walk mid-session largely prevented the decline.
By The Numbers
9–11 hrs
Average daily sitting time for office workers, including commute
30 min
Time before measurable vascular changes in seated position begin
10 min
Walk duration shown to largely reverse femoral artery dilation loss from 3 hours of sitting
2–4°C
Cooler than core temp — required for optimal testicular function
That's a remarkable finding. The damage isn't inevitable, and the reversal doesn't require a gym membership or an hour of cardio. It requires interruption. The body's vascular system is highly responsive to movement cues, even brief ones. The problem most men face isn't that they sit — it's that they sit without interruption for 2, 3, 4 hours at a stretch. That's where the compounding harm occurs.
If you work a standard desk job and drive to and from the office, it's entirely realistic that you're sitting for 9 to 11 hours on a given weekday. Add an evening of television or gaming and you're looking at a near-total absence of movement signals for your vascular system during waking hours. The "active commute" and "weekend warrior" model doesn't adequately compensate for that volume of sedentary time, according to research on sedentary behavior and cardiovascular markers.
One important clarification: this is about uninterrupted sitting, not total daily sitting. A man who sits for 8 hours but breaks it up every 30–45 minutes with standing, walking, or movement shows a markedly different vascular profile than a man who logs the same 8 hours in two uninterrupted blocks. The cumulative load matters, but the pattern matters too.
The Desk Job and Accelerated Vascular Aging
Vascular health declines with age. That's not news. What is underappreciated is the degree to which lifestyle accelerates or decelerates that timeline. The endothelium ages. Vessel walls stiffen. Nitric oxide production drops. These are normal processes — but chronic sitting appears to fast-track them, particularly in men who are otherwise healthy and assume they don't have a problem.
A 2019 study in the Journal of the American College of Cardiology tracked sedentary time independent of exercise levels and found that men with high sedentary hours showed measurably worse vascular function than active men even after controlling for total weekly exercise. In other words, the hours you spend stationary aren't neutralized by the hour you spend in the gym. They're their own independent variable. Sitting is, as some researchers have framed it, a distinct physiological state — not simply the absence of exercise.
The implications for long-term genital health are real. Arterial stiffness and reduced endothelial function are among the earliest and most reliable predictors of erectile difficulties. They show up years before most men notice clinical symptoms. A 35-year-old with 10 years of uninterrupted desk work behind him may have the vascular age of a man a decade older in the pelvic region — even if his weight, diet, and fitness routine look reasonable on the surface.
The American Heart Association has published extensive guidance on sedentary behavior and cardiovascular risk. Their position statements make clear that movement volume throughout the day — not just formal exercise — is a key determinant of vascular health. You can review their latest recommendations at the American Heart Association's Sitting Less resource hub, which covers the physiology of sedentary risk in accessible, evidence-based terms.
Posture, Chair Design, and What Makes It Worse
Not all sitting is equal. The angle of your hips, the surface you're sitting on, and the duration all combine to determine how much mechanical stress your pelvic vasculature absorbs. A few variables worth understanding:
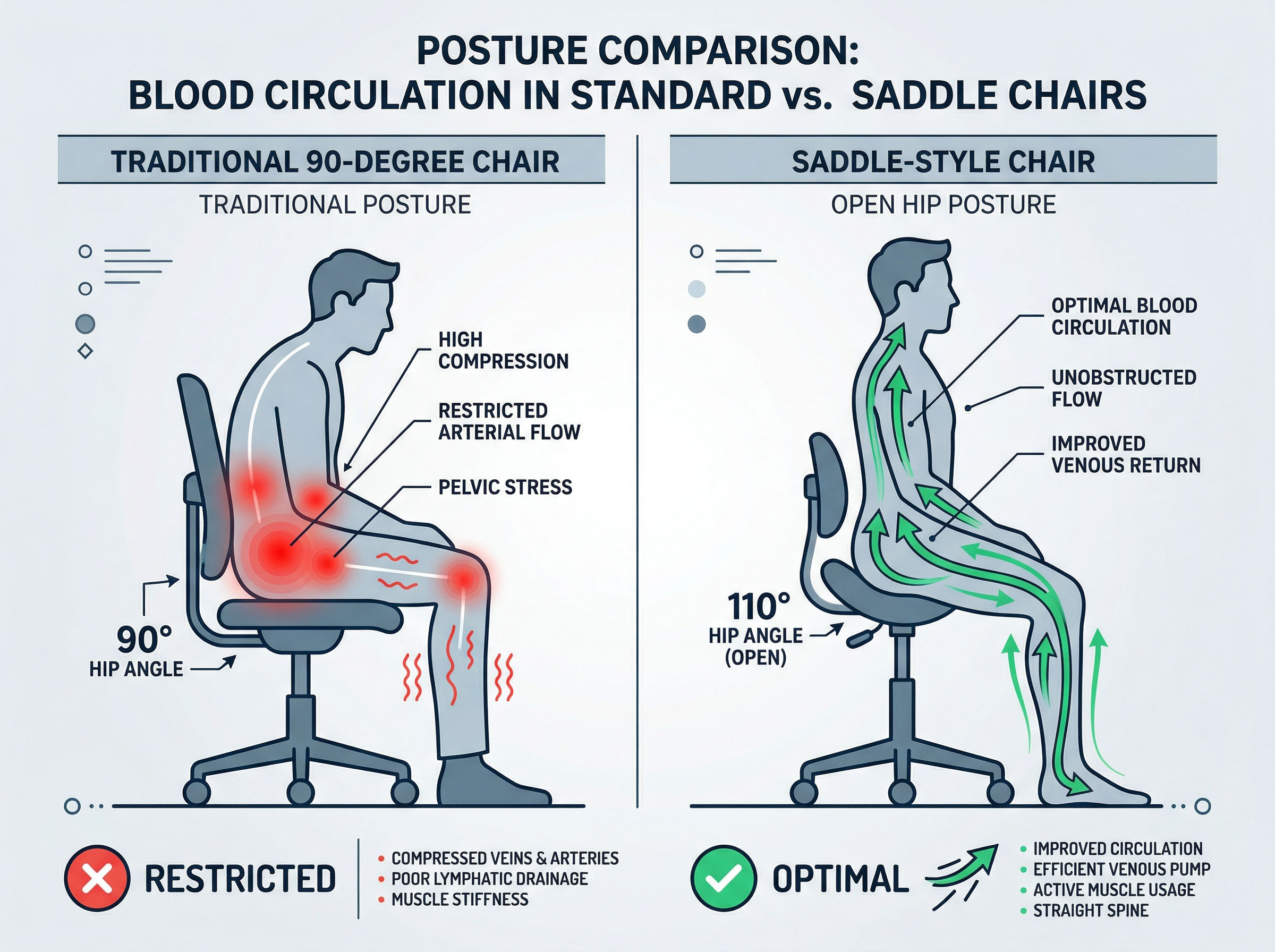
Hip flexion angle: Sitting at 90 degrees or greater (where the thigh is parallel to the floor or drops below it) creates the most compression at the femoral crease. Reclined positions — where the trunk leans back and the hip angle opens up — dramatically reduce that compression. A seat with a slight forward tilt (saddle-style or anterior-tilt chairs) also opens the hip angle and reduces perineal pressure.
Seat surface hardness: Firm, flat seat pans concentrate pressure on the perineum. Ergonomic chairs with contoured, padded, or cut-out seat pans distribute weight to the ischial tuberosities (sit bones) rather than the soft tissue between them. This is not a trivial distinction — clinical studies using pressure mapping in cyclists (who experience extreme perineal compression) confirm that surface geometry significantly affects pudendal blood flow.
Crossed legs: Crossing one leg over the other shifts the pelvis and further compresses one side's femoral vessels while also altering spinal alignment. It's a common habit that compounds whatever baseline restriction is already present from the sitting position itself.
Tight clothing: Constrictive waistbands, tight trousers, and compression around the upper thigh all contribute to restricted venous return from the lower extremities. This creates a backpressure effect in the pelvic venous system and elevates scrotal temperature.
The Commute Makes It Worse
Most analyses of occupational sitting don't fully account for commute time — but they should. A man who sits for 8 hours at a desk and then commutes an hour each way in a car seat has logged 10 hours of continuous interrupted sitting before he even reaches his front door. Car seats, almost universally, have poor hip geometry: they place the thighs roughly parallel to the floor or lower, they often have inadequate lumbar support pushing the pelvis into posterior tilt, and they hold the body in place with a seatbelt — reducing even the minor fidgeting that would otherwise provide slight relief.
Transit commuters aren't necessarily better off. Subway and bus seats vary widely in design, and standing in a moving vehicle with a neutral posture is harder than it sounds. Train riders who stand do better, but most opt for seats when available.
The point is that when you calculate true sedentary load — desk plus commute plus evening — the picture is often much worse than men assume. Most men mentally account for their gym time and feel covered. They're not accounting for the 10-plus hours their pelvis spent compressed.
⚡ Quick-Start: Desk Job Circulation Protocol
The 30/10 Rule
Every 30 minutes of sitting: stand up for 2 minutes and walk for at least 2–3 minutes. Set a timer. This is not optional if you're serious about pelvic circulatory health.
Tools Worth Using
- Standing desk or desk converter (target: 2–3 hours standing per workday)
- Saddle-style or anterior-tilt office chair (opens hip angle)
- Anti-fatigue mat for standing periods
- Under-desk walking pad (low-speed walking during calls)
- Timer app or wearable movement reminder (Apple Watch, Garmin move alerts)
Do This
- Walk during phone calls — every call is a mobility opportunity
- Take stairs, park at the far end, get off transit one stop early
- Eat lunch away from your desk and on your feet when possible
- Add hip flexor stretches and deep squat holds to your morning routine
- Consider looser-fit workwear — trapped heat and compression are cumulative
Don't Do This
- Don't assume your morning workout cancels out 9 hours of sitting
- Don't cross your legs for extended periods
- Don't rely on "I'll stretch tonight" — the vascular window is real-time
- Don't sit in a reclined-but-unmoving position and call it "relaxing" — passive slouch still restricts flow
What Good Movement Actually Looks Like
The solution to desk-job circulation problems isn't simply "exercise more." That framing sends men straight to adding another gym session, which doesn't address the pattern of the problem. The actual fix is about movement frequency and distribution — breaking up the sedentary periods, not just bookending them with intense activity.
Here's the principle behind it: your vascular system responds to shear stress — the mechanical force that blood flow exerts on vessel walls. When you move, your heart rate rises slightly, cardiac output increases, and blood moves through your vessels with more force. This stimulates endothelial cells to produce nitric oxide and maintains their health and responsiveness. When you stop moving for extended periods, shear stress drops, NO production falls, and vessel tone degrades. Brief, frequent movement — even light walking — restores shear stress and resets the clock.
This is different from cardiovascular exercise, which works at a higher intensity and achieves different adaptations. Both matter. But the 10-minute walk every hour addresses a different physiological problem than the 45-minute run three times a week. You need both tools in the kit.
For the pelvic region specifically, targeted movement helps more than generic walking. Hip circles, deep squats, lunges, and glute bridges all engage the musculature surrounding the pelvic blood supply — moving those structures, stimulating local blood flow, and countering the shortening and inhibition that sustained sitting produces. A 5-minute routine combining these movements two or three times across a workday produces meaningful circulatory benefit, and it requires no equipment and minimal time.
For men who want to understand the science behind sedentary behavior and cardiovascular risk more deeply, the research team at the Mayo Clinic's Sitting and Health resource has a clear, evidence-based breakdown of the physiological effects of prolonged sitting and practical guidance for reducing sedentary time across the day.
Playing the Long Game
Men tend to think about their health in reactive terms. Something breaks; they fix it. But pelvic circulation doesn't break dramatically — it degrades quietly, over years, in small daily increments that don't register as symptoms until the cumulative effect becomes undeniable. The man who notices in his mid-40s that his vascular responsiveness has declined has usually been building that deficit since his early 30s, when the career grind first locked him into a desk for 50 hours a week.
The upstream opportunity is straightforward: treat your daily movement pattern as a health variable, not an afterthought. A standing desk isn't a gimmick. Walking breaks aren't lost productivity. They're maintenance for a circulatory system that, left to degrade, will cost you in ways that aren't easily reversed. The men who perform well physically and sexually well into middle age are not doing anything extraordinary — they're simply not making the ordinary mistake of sitting still for a decade and expecting the machinery to stay sharp.
Your body keeps a precise account of what you put it through. The desk job syndrome is real, the mechanism is well-documented, and the prevention is unsexy but effective. Get up. Move. Do it regularly. Your pelvic circulation — and everything downstream of it — will repay the investment.
"The men who perform well physically and sexually well into middle age are not doing anything extraordinary — they're simply not making the ordinary mistake of sitting still for a decade."
— Marcus Alcott📋 In Brief
- Prolonged sitting compresses femoral vessels and the pudendal artery, reducing blood flow to the male pelvic region.
- Low shear stress from inactivity suppresses nitric oxide production — the key trigger for healthy vascular dilation.
- Testicular heat buildup from sustained sitting affects temperature-sensitive reproductive and hormonal function.
- A 10-minute walk mid-session largely reverses femoral artery dilation loss from 3 hours of sitting.
- Gym exercise doesn't cancel out hours of unbroken sedentary time — frequency of movement is what drives vascular health.
- Chair design, posture, hip angle, and clothing all modify how much pelvic compression you experience while seated.
- The solution is movement distribution throughout the day — not just more exercise volume.
Q&A: What Men Ask About Desk Jobs and Pelvic Circulation
I work out every day. Does sitting really still matter?
Yes — and this is one of the most important points in the research. Daily exercise and high sedentary time are independent variables. Studies have shown that men with high activity levels but also high uninterrupted sitting time show worse vascular markers than men with moderate activity but frequent movement breaks. Your morning workout improves cardiovascular fitness and overall health, but it doesn't counteract the physiological effect of 9 hours of immobility on pelvic blood flow. Both variables need to be managed.
How quickly can pelvic circulation be affected by sitting?
Faster than most men expect. Research using Doppler ultrasound has demonstrated measurable reductions in femoral artery dilation within 30–60 minutes of continuous sitting. After 3 hours, the reduction is significant in otherwise healthy young men. The good news: the recovery is equally fast. A 10-minute walk restores a significant portion of flow-mediated dilation, which means the window for intervention is always close.
Does a standing desk actually help?
Yes, with caveats. Standing relieves perineal and femoral compression, and promotes more natural posture. But prolonged static standing has its own drawbacks — increased venous pooling in the legs, lumbar load, and fatigue. The evidence supports alternating between sitting and standing, aiming for roughly 2–3 hours of standing across a workday, broken into segments. The key word is movement — a standing desk is most effective when it's part of a pattern that also includes walking, rather than simply replacing one static position with another.
Are there specific exercises that target pelvic circulation?
Several movements directly improve blood flow to the pelvic region: hip circles, deep squats, glute bridges, reverse lunges, and hip flexor stretches all engage the muscles surrounding the major pelvic vessels and the pelvic floor itself. These movements counter the shortening and inhibition that sitting produces in the hip flexors and glutes. A 5–8 minute routine using these movements 2–3 times across a workday — not just at the gym — provides meaningful circulatory benefit. Walking is also highly effective due to the rhythmic activation of the glutes and hip flexors, which acts as a mechanical pump on the pelvic vasculature.
What chair setup is best for minimizing pelvic compression?
Look for three things: an open hip angle (greater than 90°, achievable with a forward-tilted or saddle-style seat), a contoured seat pan that distributes weight to the sit bones rather than the soft tissue of the perineum, and adequate seat padding. Chairs with a cut-out or waterfall front edge also reduce compression on the underside of the thighs. Adjusting seat height so your feet are flat on the floor and your hips are at or slightly above knee level helps maintain a better pelvic position. No chair eliminates the need to stand up and move — but the right setup meaningfully reduces the per-minute mechanical load.
Disclaimer: The articles and information provided by Genital Size are for informational and educational purposes only. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition.


 日本語
日本語  Deutsch
Deutsch  English
English  Español
Español  Français
Français  Português
Português