10 Facts Most Men Don't Know About Their Own Anatomy

10 Facts Most Men Don't Know About Their Own Anatomy
Most men can name the parts. Few actually understand how they work. The standard health curriculum handed to boys covers the basics and moves on, leaving a surprising number of adult men carrying outdated assumptions — or outright myths — about their own bodies. That's not a small problem.
Understanding your anatomy isn't vanity; it connects directly to reproductive health, self-awareness as a father, and the kind of confidence that comes from knowing what's actually going on under the hood.
This isn't a clinical lecture. Think of it as the briefing you should have gotten but didn't. Here are ten facts that are genuinely surprising, scientifically grounded, and worth knowing — whether you're planning a family, managing your health, or simply tired of operating blind on something this fundamental.
In Brief
- Most men have never been taught the real mechanics of their own reproductive anatomy.
- Genital anatomy is more complex — and more interesting — than locker-room myths suggest.
- Understanding your body directly affects reproductive health, confidence, and informed decision-making.
- This article covers 10 science-backed facts that most men were never told.
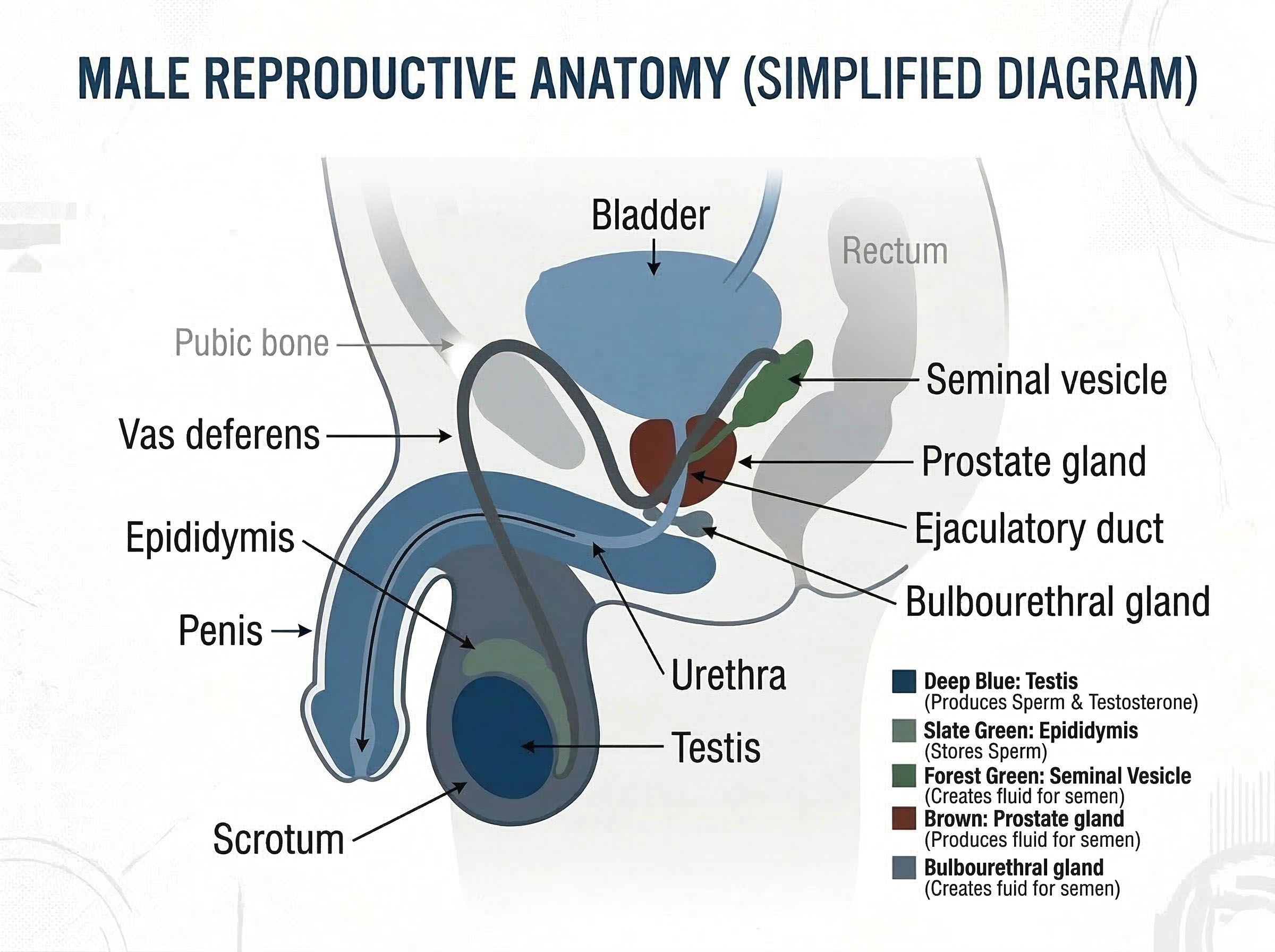
Understanding your anatomy is the foundation of informed reproductive health decisions.
1. The Penis Is Mostly Internal
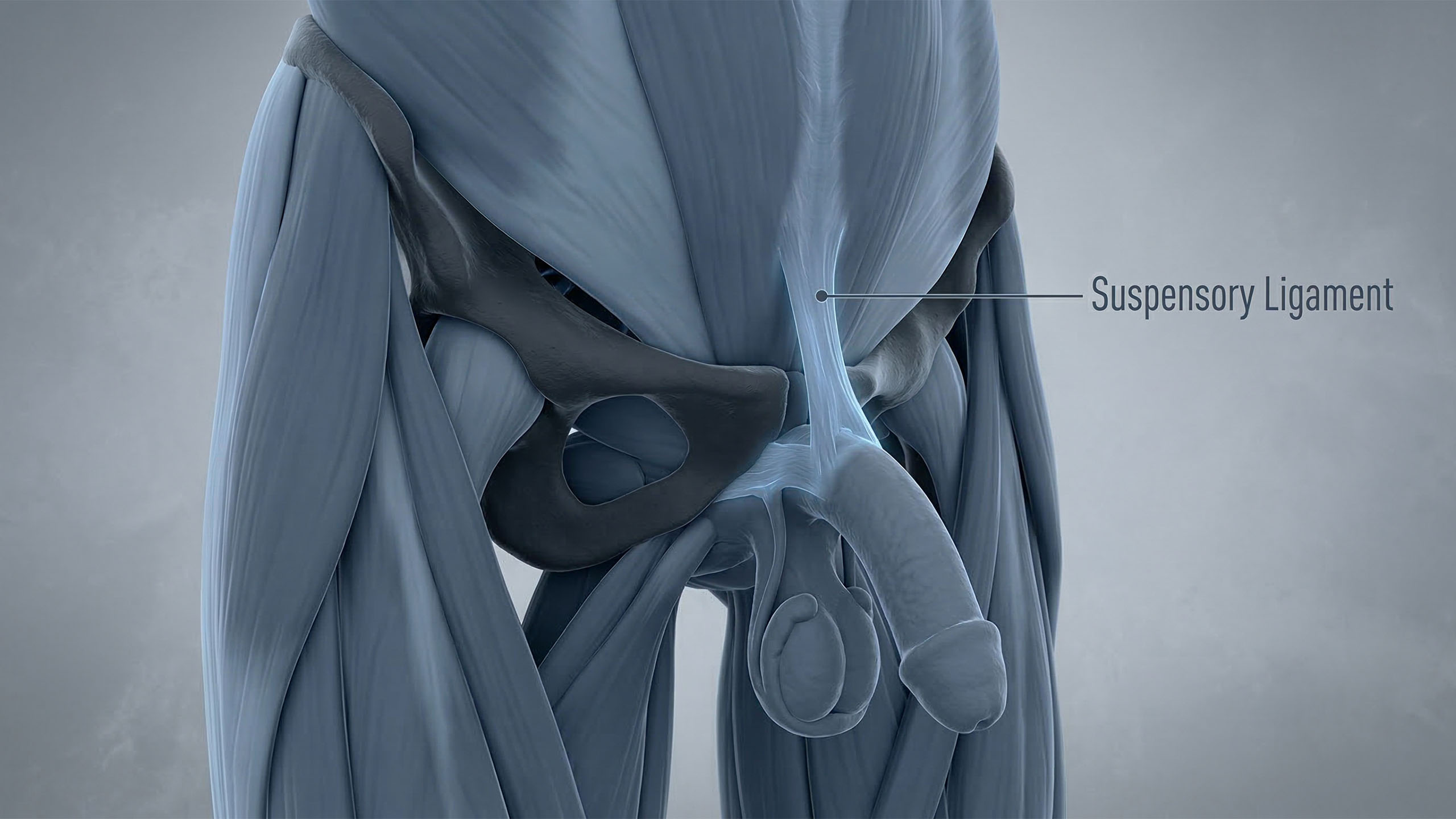
Here's the one that stops most men cold. What you see externally is only a portion of the full organ. The root of the penis — called the radix — extends internally into the perineum and pelvis, attached to the pubic arch via structures called the crura and the bulb of the penis. In some anatomical studies, the internal portion accounts for roughly one-third to nearly half of the total penile length. The full internal structure wraps around the urethra, anchors to bone and connective tissue, and plays a direct role in erection mechanics. This isn't trivia — it explains why things like body weight and pelvic floor health can visibly affect external appearance and function.
"What you see is only part of the story. The root of the penis anchors internally — and that internal structure matters more than most men realize."
— Adrian Lowe
2. Erections Happen Without You — Starting Before Birth
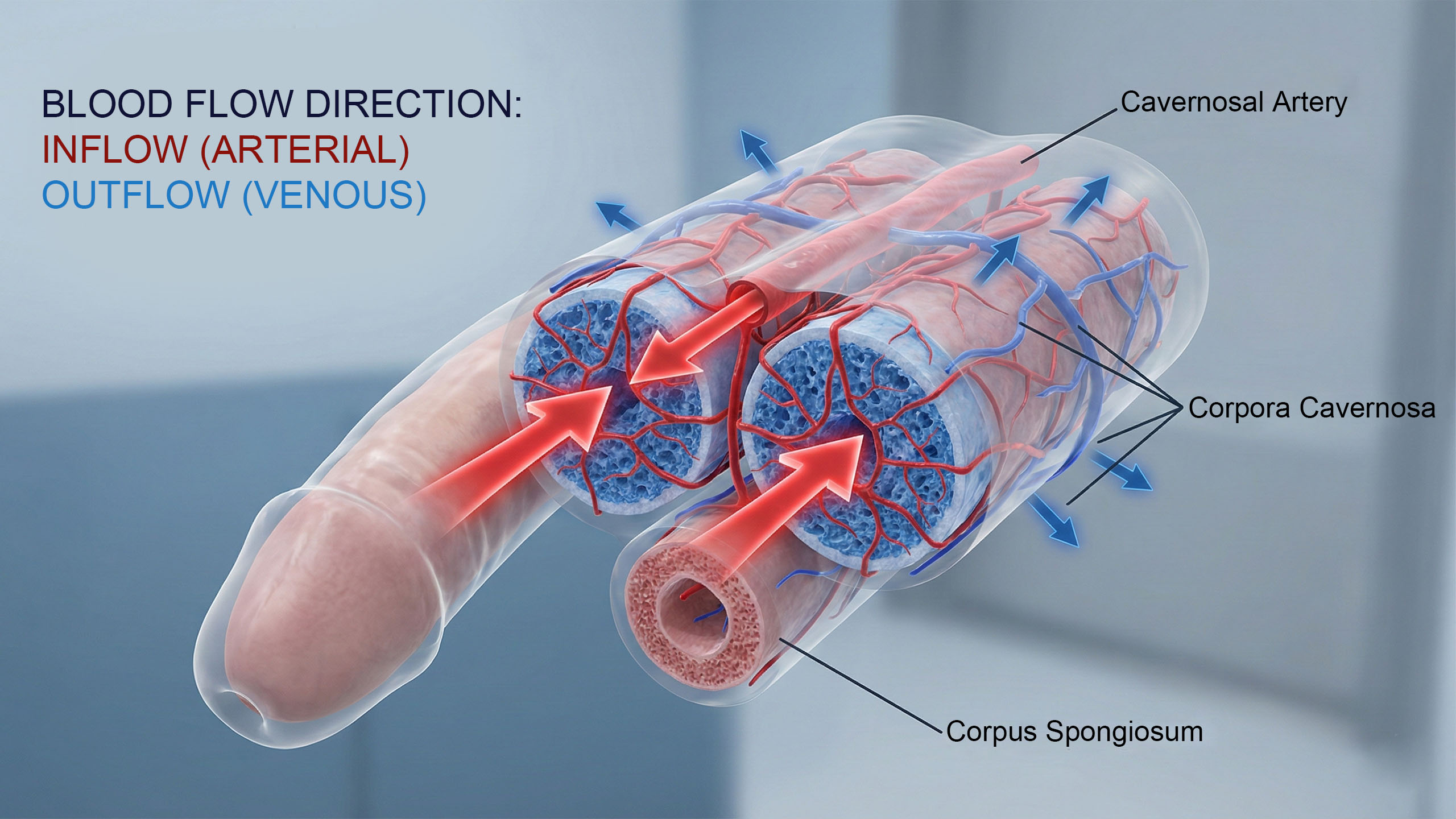
Male fetuses experience erections in the womb. This has been documented via ultrasound and is entirely reflexive — a sign that the vascular and neurological systems involved in erection are functional and developing normally. The same reflex continues through infancy and childhood, long before any sexual context exists. Nocturnal erections — the ones that occur during REM sleep throughout a man's life — serve a physiological purpose: they maintain oxygenation of penile tissue. Men average three to five of these per night. When they stop occurring, it's often one of the earliest indicators of cardiovascular or hormonal changes worth investigating. The body maintains its own maintenance schedule, whether you're paying attention or not.
3. Sperm Takes Over Two Months to Develop
Sperm production — spermatogenesis — is not an on-demand process. A single sperm cell takes approximately 64 to 74 days to develop from a primitive germ cell to a mature, motile sperm capable of fertilization. Add another 12 to 21 days of transit time through the epididymis where sperm matures and gains motility, and you're looking at roughly three months from start to finish. This matters practically: anything that affects your health today — illness, medications, heat exposure, alcohol consumption — is affecting the sperm that will be viable three months from now. For men planning to conceive, the preparation timeline isn't measured in weeks. It's measured in months.
Did You Know?
The average male produces roughly 1,500 sperm every second. Over a lifetime, that adds up to hundreds of billions of cells — making the testes one of the most metabolically active tissues in the human body.
4. Testicle Size and Sperm Count Are Not the Same Thing
Larger testicles do tend to correlate with higher sperm production — but the relationship is not as direct as men assume, and size tells you almost nothing about sperm quality. Motility (how well sperm swim), morphology (whether sperm are correctly shaped), and DNA fragmentation are the metrics that actually predict fertility outcomes. A man with average-sized testicles and high-quality sperm will typically outperform a man with larger testicles and poor motility in a fertility context. If reproductive health is a concern, a semen analysis — not a mirror — is the appropriate diagnostic tool.
5. The Foreskin Is a Functional Structure
Regardless of whether a man is circumcised or not, understanding what the foreskin actually does is useful anatomy. In intact males, the foreskin — or prepuce — serves as a protective covering for the glans, keeps mucosal tissue from keratinizing (thickening and desensitizing through constant air and friction exposure), and contains a concentration of specialized nerve endings including Meissner's corpuscles. It also plays a role in the mechanical dynamics of intercourse by reducing friction. Circumcision rates vary widely by country — common in the United States for both cultural and historical medical reasons, far less so in Europe and much of Asia. Neither state is a health deficiency. Knowing the anatomy either way is simply useful.
Cultural Insight
Circumcision Around the World
In the United States, neonatal circumcision became widespread in the early 20th century, partly driven by health theories of that era. In Western Europe, Scandinavia, and East Asia, circumcision is uncommon outside of religious practice. In parts of sub-Saharan Africa and the Middle East, it holds deep cultural and religious significance. The World Health Organization estimates roughly 37–39% of men globally are circumcised. Cultural context — not universal medical consensus — drives the majority of these differences.
6. The Scrotum Is a Temperature-Control System
Sperm production requires a core temperature roughly 2 to 4 degrees Celsius below normal body temperature — which is why the testes are housed externally rather than inside the body cavity. The scrotum isn't simply a container. It is a dynamic thermoregulatory system. The cremaster muscle raises and lowers the testes in response to temperature changes. The dartos muscle causes the characteristic wrinkling of scrotal skin, which increases or decreases surface area for heat exchange. When cold, the scrotum contracts and pulls the testes closer to the body for warmth. When warm, it relaxes and drops them lower for cooling. Prolonged heat exposure — from hot tubs, laptops placed directly on the lap, or sedentary desk work in tight clothing — has been shown in multiple studies to temporarily reduce sperm quality. The system works, but only if you're not consistently overriding it.
| Factor | Effect on Sperm | Approx. Recovery Time |
|---|---|---|
| Fever (38°C+) | Reduced motility, morphology | ~3 months |
| Prolonged heat exposure (hot tubs, saunas) | Temporary count reduction | 6–12 weeks |
| Heavy alcohol use | Morphology and DNA integrity | ~3 months |
| Anabolic steroids (exogenous testosterone) | Severe count suppression | 6–24 months (variable) |
| Smoking | Motility and DNA fragmentation | ~3 months post-cessation |
| Stress / poor sleep | Hormonal disruption, count | Weeks to months |
Note: Recovery timelines are general estimates. Individual outcomes vary. Consult a urologist or reproductive specialist for personal health concerns.
7. The Prostate Is More Than a Gland Men Worry About After 50
The prostate gland gets discussed almost exclusively in the context of cancer screening — which is important, but limits men's understanding of what it actually does. The prostate is a walnut-sized gland wrapped around the urethra, just below the bladder. Its primary function is to produce a fluid that makes up roughly 25 to 30 percent of the total volume of semen. This fluid is slightly alkaline, which helps neutralize the acidic environment of the vagina, protecting sperm during transit. The prostate also plays a role in the mechanics of ejaculation by contracting at the point of orgasm. It contains smooth muscle tissue that pushes prostatic fluid into the urethra and contributes to the force of ejaculation. It's an active participant in reproduction — not a passive bystander that only becomes relevant when something goes wrong.
Worth Knowing
The prostate can be assessed by a doctor through a digital rectal exam (DRE) or PSA blood test. Current guidelines generally recommend discussing prostate screening with a doctor starting at age 50 — or 40 to 45 for men with a family history of prostate cancer or those of African descent, who face higher statistical risk.
8. Penile Length Has Almost No Statistical Relationship to Shoe Size, Height, or Hand Size
This one has been studied, confirmed, and largely ignored by popular culture. Multiple peer-reviewed studies — including a frequently cited 2015 study published in the BJU International journal involving over 15,000 men — have found that correlations between penile size and other body measurements are either negligible or statistically insignificant. Height, shoe size, finger length: none are reliable predictors. The same studies documented average flaccid length at approximately 9.16 cm (3.6 inches) and average erect length at approximately 13.12 cm (5.16 inches). Knowing the actual numbers — rather than the inflated figures that dominate male perception — matters because male anxiety about size is disproportionate to actual variation in the general population, and that anxiety has real effects on confidence, relationships, and even help-seeking behavior.
9. Varicoceles Are Extremely Common — and Frequently Undiagnosed
A varicocele is an enlargement of the veins within the scrotum — similar in concept to varicose veins in the legs. They occur in approximately 15 percent of all men and in roughly 35 to 44 percent of men investigated for primary infertility. They are the most common correctable cause of male infertility. Despite this prevalence, most men have never heard the term. Varicoceles are typically painless (though some men experience a dull ache, especially after standing for long periods), develop most commonly on the left side due to the angle at which the left testicular vein drains, and are detectable through physical examination or scrotal ultrasound. Left untreated, they can cause progressive testicular atrophy and declining sperm parameters over time. They are also surgically correctable with a relatively straightforward procedure. The only barrier to addressing them, for most men, is knowing they exist.

Conditions like varicoceles are common, correctable — and almost entirely unknown to most men.
10. Male Fertility Declines With Age — It Just Does So More Slowly Than Female Fertility
The cultural assumption is that men remain fully fertile indefinitely. The reality is more measured. Sperm quality — including motility, morphology, and DNA integrity — begins a gradual decline starting around age 40 to 45. Studies have linked advanced paternal age (generally defined as 40 and above) to modest increases in certain chromosomal abnormalities, miscarriage rates in partners, and specific developmental conditions in offspring. The changes are incremental, not cliff-like, and men routinely father healthy children well into their 50s and beyond. But the assumption of unlimited reproductive time is not accurate. Testosterone levels also typically decline by roughly one to two percent per year beginning in a man's 30s — a process called andropause or late-onset hypogonadism — which affects energy, mood, muscle mass, and libido, though it rarely receives the same cultural attention as female menopause.
Quick-Start: What to Actually Do With This Information
Tools & Resources
- Request a semen analysis from a urologist or reproductive clinic — it's the only way to know your actual sperm parameters.
- Consider a scrotal ultrasound if you've experienced a dull ache or fertility challenges — rules out varicoceles.
- Discuss PSA testing and prostate health with your doctor starting at 40–50 depending on your risk profile.
Do's
- Wear loose-fitting underwear if fertility is a current concern — scrotal temperature management is real.
- Give yourself a 90-day clean window before a fertility attempt: minimize alcohol, heat exposure, and high stress where possible.
- Understand your family history of prostate conditions — it directly informs your screening schedule.
- Talk openly with your doctor. Male reproductive health visits are underutilized — and that has real consequences.
Don'ts
- Don't assume exogenous testosterone (TRT or steroids) has no fertility cost — it can severely suppress sperm production.
- Don't use laptop heat on the lap for hours daily if you're trying to conceive.
- Don't skip annual physicals because you feel fine. Most male reproductive conditions are asymptomatic until they're not.
The Bigger Picture
There's a certain kind of man who figures he doesn't need to know how his body works unless something breaks. That posture costs more than most men realize — in delayed diagnoses, in fertility windows missed, in anxiety built on myths that a five-minute conversation with real information could dismantle. Your anatomy is not complicated. But it is real, and it is worth understanding.
The ten facts above are not edge cases. They are foundational. Whether you're a father already or planning to be one, whether you're 25 or 55, knowing how your body actually operates is the first step in taking care of it properly. That's not a soft idea — it's a practical one. And it starts with being willing to look at what's actually there.
Frequently Asked Questions
Does penile size affect fertility?
No. Penile size has no measurable relationship to sperm count, sperm quality, or the ability to conceive. Fertility is determined by sperm parameters — motility, morphology, count, and DNA integrity — none of which correlate with external size. A semen analysis is the appropriate way to assess fertility potential.
How long should a man abstain before a fertility test or attempt to conceive?
Standard guidance for semen analysis is two to five days of abstinence before the sample is collected, to ensure an accurate count. For maximizing sperm quality for conception, longer abstinence does not improve outcomes — in fact, very long periods of abstinence can reduce motility. Regular ejaculation (every two to three days) during a fertile window is generally considered optimal.
At what age should men start thinking about prostate health?
General guidelines recommend discussing prostate screening with a doctor at age 50 for average-risk men. Men with a father or brother who had prostate cancer, or men of African descent (who face statistically higher risk), should begin this conversation at age 40 to 45. Prostate conditions are highly treatable when detected early — the barrier is usually awareness and willingness to bring it up.
Can a man fully recover fertility after using anabolic steroids?
Recovery is possible for many men, but it is not guaranteed and can take anywhere from several months to over two years depending on duration of use, compounds used, and individual biology. Exogenous testosterone suppresses the hypothalamic-pituitary-gonadal axis, which regulates natural testosterone and sperm production. Recovery protocols exist but results vary widely. Men planning to father children should factor this in before beginning any hormone protocol.
Is one testicle hanging lower than the other normal?
Yes — this is entirely normal and experienced by the vast majority of men. The left testicle typically hangs slightly lower than the right due to the anatomy of the spermatic cords. The asymmetry is a design feature, not a defect — it allows the testes to move independently for thermoregulation without compressing each other. Any sudden change in size, persistent pain, or the appearance of a lump, however, warrants a prompt medical evaluation.
Disclaimer: The articles and information provided by Genital Size are for informational and educational purposes only. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition.


 日本語
日本語  Deutsch
Deutsch  English
English  Español
Español  Français
Français  Português
Português